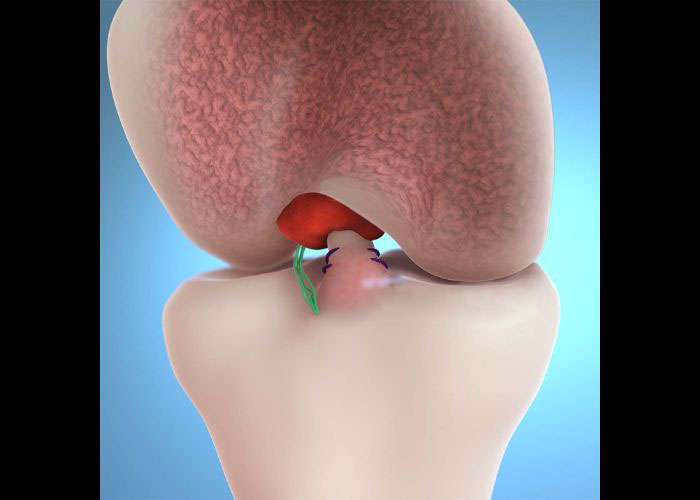
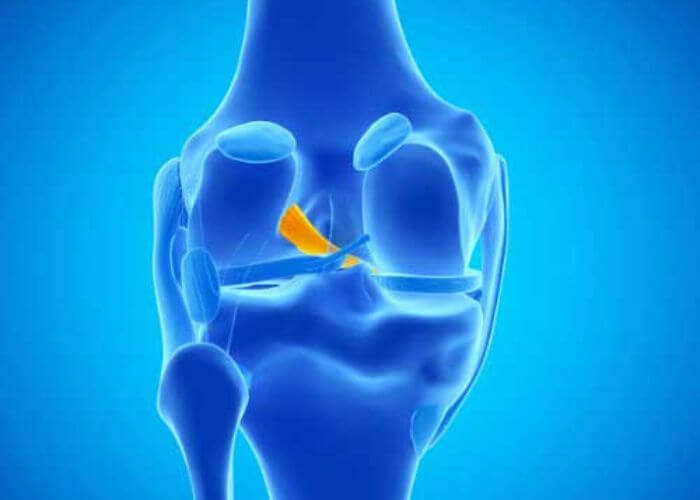
What is a posterior cruciate ligament (PCL) injury?
There are two cruciate ligaments that form an “X” within the knee joint and work collectively to limit the forward and backward movement of the tibia (shin bone) in relation to the femur (thigh bone). The posterior cruciate ligament (PCL) originates on the posterior femur and crosses behind the anterior cruciate ligament (ACL) to attach to the anterior tibia. Approximately the size of one’s little finger, the PCL has two segments that join to form the strongest of the four main knee ligaments. This ability to withstand a significant stress load makes the PCL the least injured of the knee ligaments; however, a substantial force on the anterior shin and knee can stretch or tear the PCL from its attachment site. Athletes involved in aggressive contact sports, such as football, rugby, or wrestling, have the highest likelihood of sustaining a PCL injury. Non-athletic individuals can still damage the PCL in the event of a motor vehicle collision or a fall directly onto a bent knee. Dr. Ronak Mukesh Patel, orthopedic knee specialist serving patients in Sugar Land, Pearland, and the Houston, Texas area, has the knowledge and understanding as well as substantial experience in treating patients who have experienced a posterior cruciate ligament injury.
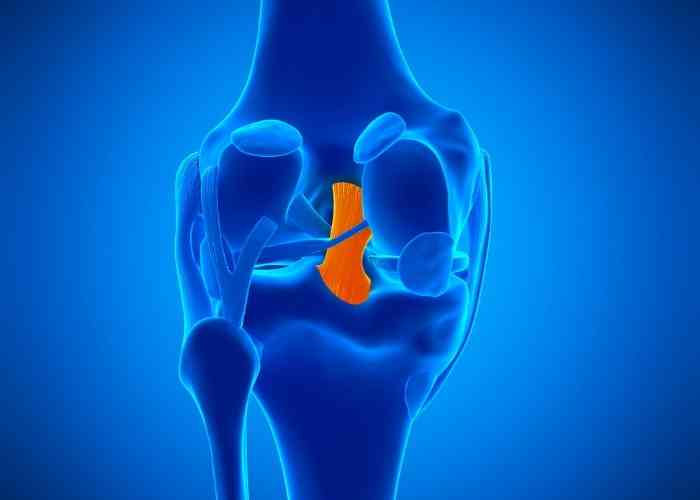
Are there varying degrees of a posterior cruciate ligament injury?
The criteria for grading posterior cruciate ligament (PCL) injuries involve assessing the severity of damage and classifying them into three categories:
- Grade 1 injury: Shows minimal damage from the ligament being pulled or stretched.
- Grade 2 injury: Occurs when the ligament is stretched beyond its limits resulting in a partial tear from the attachment site.
- Grade 3 injury: Results in knee joint instability from a complete rupture of the ligament into two separate pieces.
What are the symptoms of a posterior cruciate ligament injury?
Because of the amount of force needed to cause damage to the posterior cruciate ligament (PCL), it is rarely the only knee ligament affected in a traumatic event. Individuals with a suspected PCL injury report pain and instability of the knee. Swelling of the affected knee can also occur especially with continued physical activity. Some other common symptoms of a PCL injury can include difficulties with certain movements such as:
- Twisting or pivoting the affected lower leg
- Walking downstairs or slowing down on a run
How is a posterior cruciate ligament injury diagnosed?
A comprehensive medical history, with a focus on prior knee injuries and conditions, will be gathered through an interview with Dr. Patel. A thorough physical examination will follow involving a series of orthopedic tests to assess stability of the affected knee and careful testing of all knee ligaments. Diagnostic imaging studies are particularly useful for suspected posterior cruciate ligament (PCL) injuries. X-rays can identify if any bone-related damage occurred as a result of the precipitating injury. Magnetic resonance imaging (MRI) can identify the extent of damage to the PCL as well as evaluate the surrounding soft tissue structures for any additional damage.
What is the treatment for a posterior cruciate ligament (PCL) injury?
Non-surgical treatment:
If the posterior cruciate ligament (PCL) was the only ligament that sustained damage, conservative therapies may alleviate any associated symptoms. Avoiding or limiting weight-bearing can prevent further injury to the knee joint. A combination of RICE (rest, ice, compression, elevation) and non-steroidal anti-inflammatory medications (NSAIDs) is encouraged for pain and inflammation management. Participating in a physical rehabilitation program is crucial for repairing damage to the PCL.
Surgical treatment:
More often, however, there is damage to other ligaments or structures of the knee joint which necessitates surgical reconstruction of the posterior cruciate ligament (PCL) and all other ligaments to properly restabilize the knee joint. A minimally invasive arthroscopic procedure involving a small camera (arthroscope) and specialized surgical instruments removes the damaged tissue fragments. If enough healthy tissue remains, the PCL is simply reattached in the correct anatomical position. A complete rupture of the PCL will often utilize a tissue graft, either from the patient (autograft) or donor (allograft), for new tissue to generate. This new ligament is passed through a tunnel within the head of the tibia and fastened to the femur with special surgical anchors.
PCL Injury Specialist

The posterior cruciate ligament (PCL) forms an “X” with the ACL or anterior cruciate ligament within the knee joint. Damage to the PCL can cause difficulty with twisting or turning movements, or with walking down stairs. PCL injury specialist, Doctor Ronak Mukesh Patel, provides diagnosis as well as surgical and nonsurgical treatment options for patients in Houston, Sugar Land, and Pearland, TX who have injured their PCL. Contact Dr. Patel’s team today!